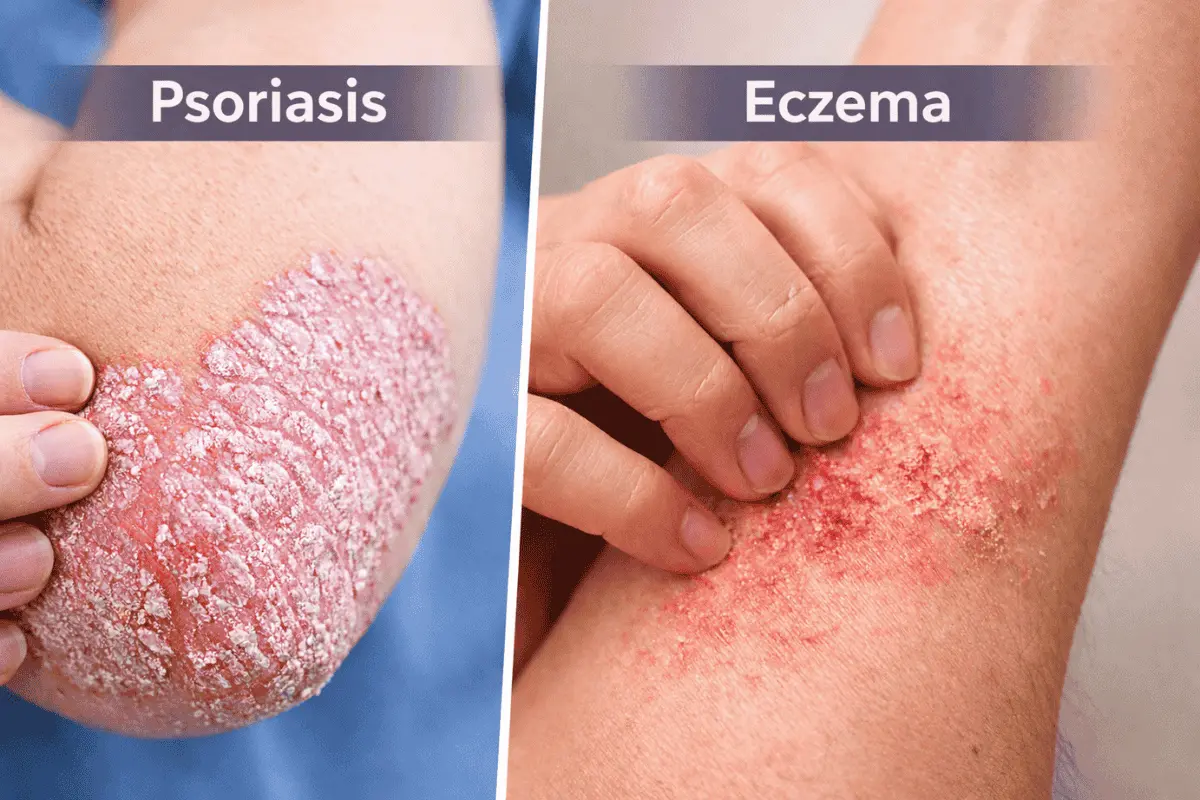
Skin conditions can be hard to identify on your own. Two of the most commonly confused conditions are psoriasis and eczema. Understanding the differences between psoriasis vs eczema is important, as both can cause redness, itching, and dry skin, making them easy to confuse. They are distinct conditions, nevertheless, with different origins and treatment methods.
Understanding the difference between psoriasis vs eczema matters because the wrong treatment can worsen symptoms. A correct diagnosis gives you a much better chance of finding relief faster.
This article clearly and simply breaks down the key differences, covering symptoms, causes, body locations, and treatment options.
What Is Psoriasis?
Psoriasis is a chronic immune-mediated disease. The immune system becomes overactive, speeding up the skin cell growth cycle. Normally, skin cells grow and shed over about a month. In the case of psoriasis, that process takes only three to four days. The skin cells pile up on the surface because the body cannot shed them fast enough.
According to the National Psoriasis Foundation, psoriasis is not contagious and affects about 3% of adults in the United States.
Common Symptoms of Psoriasis
- Thick, raised patches of skin called plaques
- Silvery-white or scaly coating on the skin
- Dry skin that may crack or bleed
- Itching, burning, or stinging
- Changes to nails, including small dents or discolouration
The itch with psoriasis tends to vary. Some people feel a mild itch, while others describe more of a burning or stinging sensation.
Common Types of Psoriasis
- Plaque psoriasis is the most common type and accounts for about 80 to 90 percent of cases. It causes well-defined, thick red patches covered with silvery scales, most often on the elbows, knees, and scalp.
- Guttate psoriasis causes small, salmon-colored bumps that often appear suddenly, usually on the torso, arms, and legs. It tends to develop in children and young adults following a bacterial infection such as strep throat.
- Inverse psoriasis develops in skin folds, such as the armpits or the groin. The patches look smooth and raw rather than scaly.
- Pustular psoriasis causes pus-filled bumps that usually appear on the hands and feet. Despite how it looks, the skin is not infected.
What Is Eczema?
Eczema, also called atopic dermatitis, is a condition that causes dry, itchy, and inflamed skin. It is the most common type of eczema and is closely linked to allergies and a weakened skin barrier. Some people with atopic dermatitis have a mutation in the filaggrin gene, which makes the skin less able to hold moisture and more vulnerable to irritants and allergens.
Unlike psoriasis, eczema is driven by a different type of immune response, one closely tied to allergic inflammation.
Common Symptoms of Eczema
- Intense itching, often worse at night
- Dry, cracked, or scaly skin
- Red, inflamed patches with less defined borders
- Oozing or crusting in some cases
- Thickened skin in areas that are scratched frequently

The itch associated with eczema tends to be more intense than with psoriasis. Dr Paul Yamauchi, a dermatologist at the Dermatology Institute and Skin Care Centre in Santa Monica, noted that “eczema may cause an intense itch while psoriasis causes more of a burning or stinging sensation or mild itch.”
Who Is Most Likely to Get Eczema?
Eczema most often begins in childhood, frequently before age five. According to the National Psoriasis Foundation, atopic dermatitis affects more than 9.6 million children and about 16.5 million adults in the United States. People with a personal or family history of allergies, asthma, or hay fever have a higher risk of developing eczema.
Psoriasis vs Eczema: Key Differences
Appearance of the Skin
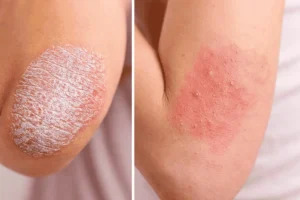
Psoriasis typically presents with well-defined, thick plaques covered in silvery scales. Dr Benjamin Ungar, director of the Alopecia Centre of Excellence at Mount Sinai, described it as: “Psoriasis tends to present with well-demarcated thick red plaques with silvery scales.”
Eczema patches tend to have less distinct borders. The skin looks more like a patchy rash, red or brown, sometimes with small bumps or crust. It generally appears thinner and less raised than psoriasis.
Location on the Body
Location is one of the clearest ways to distinguish these two conditions. Psoriasis commonly appears on the outer edges of the elbows, knees, scalp, lower back, palms, and soles. Eczema tends to appear in the skin folds, including the inner elbows, behind the knees, wrists, neck, and ankles. In babies, eczema often shows up on the cheeks, chin, and scalp.
Age of Onset
Eczema usually begins in childhood and may improve with age. Psoriasis typically first appears in adults between ages 20 and 30, with a second peak around age 60.
Causes and Triggers
Both conditions involve the immune system, but in different ways. Th1 and Th17 T-cells drive psoriasis, while eczema is primarily driven by Th2 T-cells associated with allergic inflammation. Common triggers for eczema include soaps, fragrances, wool fabrics, dust mites, pet dander, heat, and stress. Stress, skin injury, infections, certain medications, and weather changes more often trigger psoriasis flares.
| Feature | Psoriasis | Eczema |
| Primary Immune Cells | Th1 and Th17 T-cells | Th2 T-cells |
| Appearance | Thick, scaly plaques with well-defined edges | Red, inflamed skin, often dry and cracked |
| Common Triggers | Stress, skin injury, infections, medications, and weather changes | Soaps, fragrances, wool, dust mites, pet dander, heat, stress |
| Distribution | Commonly found on the scalp, elbows, and knees | Typically occurs on hands, feet, inner elbows, and behind knees |
| Onset Age | Peaks between 20-30 and around 60 | Often starts in childhood, but can occur at any age |
| Associated Conditions | Psoriatic arthritis | Asthma, hay fever |
Treatment Options
Treating Psoriasis
Treatment for psoriasis focuses on slowing skin cell growth and reducing inflammation. Options include:
- Topical treatments: corticosteroids, vitamin D analogs, salicylic acid, and newer options like roflumilast cream (Zoryve) or tapinarof cream (Vtama)
- Phototherapy: exposure to specific wavelengths of light under medical supervision
- Systemic medications: methotrexate, cyclosporine, and oral medications like apremilast
- Biologic drugs: targeted therapies that block specific immune pathways involved in psoriasis
Treating Eczema
Eczema treatment focuses on repairing the skin barrier, reducing irritation, and preventing flare-ups. Options include:
- Moisturisers: fragrance-free creams and ointments applied regularly
- Topical corticosteroids: to reduce inflammation during flares
- Topical calcineurin inhibitors: such as pimecrolimus (Elidel) and tacrolimus (Protopic)
- Newer medications: dupilumab (Dupixent), a biologic approved for moderate-to-severe atopic dermatitis, and JAK inhibitors like abrocitinib (Cibinqo) and upadacitinib (Rinvoq)
- Trigger management: identifying and avoiding specific irritants
Biologics are available for both conditions, but they are not interchangeable. A biologic that targets psoriasis will not work for eczema because each condition involves different inflammatory pathways.
When to See a Dermatologist
You should consult a dermatologist if:
- Skin symptoms persist or worsen over time
- Itching is severe enough to disrupt sleep or daily life
- You notice signs of infection, such as streaks, pus, or yellow crusting
- Over-the-counter treatments are not providing relief
A board-certified dermatologist can accurately diagnose your condition and create a treatment plan suited to your needs. Delaying a proper diagnosis often means living with unnecessary discomfort.
Living With Chronic Skin Conditions
Both psoriasis and eczema are chronic conditions without a cure, but their symptoms can be well-managed with the right approach. Maintaining a consistent skin care routine, managing stress, identifying personal triggers, and following medical guidance all make a meaningful difference.
People who mistake one condition for the other sometimes spend months using the wrong treatments. That delay can lead to more severe symptoms and, with psoriasis, a higher risk of related health conditions like psoriatic arthritis.
The Bottom Line on Psoriasis vs Eczema
Psoriasis and eczema share some surface-level similarities, but they are distinct conditions. Psoriasis involves well-defined, scaly plaques driven by a specific immune dysfunction. At the same time, eczema causes intense itching and less-defined patches, closely tied to allergic reactions and a compromised skin barrier.
Knowing the differences between psoriasis vs eczema gives you a starting point. From there, a dermatologist can confirm your diagnosis and guide you toward the most effective treatment. The sooner you get the right diagnosis, the sooner you can find real relief.
Frequently Asked Questions
Can psoriasis and eczema appear at the same time?
Yes, it is possible, though uncommon. Research has found that a small percentage of children with eczema also have psoriasis. A dermatologist can evaluate whether you have one or both conditions.
Is psoriasis vs eczema easier to diagnose in children or adults?
Eczema is more common in children and is often easier to identify given its typical locations and age of onset. Psoriasis more commonly appears in adults and may be harder to distinguish in areas like the palms, soles, or skin folds, where it does not always present with its classic silvery scale.
Can stress trigger both psoriasis and eczema?
Yes. Stress is a recognised trigger for both conditions and can cause flares or worsen existing symptoms. Stress management techniques, including regular exercise and mindfulness practices, are often recommended alongside medical treatment for both psoriasis and eczema.