Sepsis kills more Americans each year than many well-known diseases, yet most people still have only a vague understanding of what it actually is. One of the most common questions people ask after a family member or friend is diagnosed is: Is sepsis contagious? It is a fair question, and the answer matters for anyone trying to protect themselves and the people around them. Understanding how sepsis develops, what causes it, and how it behaves in the body makes it much easier to separate fact from fear.
What Is Sepsis?
The body’s severe response to an infection is sepsis. According to the CDC, it is a life-threatening medical emergency that happens when an infection you already have triggers a chain reaction throughout your body. Rather than fighting the infection in a controlled way, the immune system goes into overdrive. That overreaction causes widespread inflammation that can damage tissues, impair organ function, and, without prompt treatment, lead to death.
The infections most likely to lead to sepsis typically start in the lungs, urinary tract, skin, or gastrointestinal tract. Bacteria cause most cases, but viral and fungal infections can also trigger it.
According to the CDC, about 1.7 million adults in the United States develop sepsis each year, and at least 350,000 of them die during hospitalisation or are discharged to hospice. It is not a rare or obscure condition. It is a real public health issue.
Is Sepsis Contagious?
The quick response is no. There is no way to spread sepsis. As the CDC clearly states: “You can’t spread sepsis to other people.” The NHS echoes this directly: “You cannot catch sepsis from another person.”
The reason comes down to what sepsis actually is. By itself, sepsis is not an infection. It is the body’s abnormal response to an infection, meaning it is a condition that develops inside one individual based on how their immune system reacts. That internal reaction cannot be passed on to another person through physical contact, shared air, or bodily fluids.
That said, there is an important nuance worth understanding. While sepsis is not contagious, the underlying infection that triggered it sometimes can be. Pneumonia, for example, can spread from person to person through respiratory droplets. A urinary tract infection, on the other hand, is generally not transmissible. So the question of whether the infection itself is contagious depends entirely on what type of infection caused the sepsis in the first place.
Infections That Can Lead to Sepsis
Sepsis can follow almost any type of infection. The most common categories include:
Bacterial infections are responsible for the majority of sepsis cases. These include pneumonia, bloodstream infections, and urinary tract infections. When bacteria multiply unchecked in the body, the immune system can respond in a dangerously exaggerated way.
Viral infections can also set off the chain reaction. Severe illnesses like influenza and COVID-19 have been linked to sepsis, particularly in people with weakened immune systems.
Fungal infections are a less common but serious cause, and they tend to affect people who are immunocompromised, such as those undergoing chemotherapy or living with HIV.
How Sepsis Develops in the Body
When a harmful pathogen enters the body, the immune system launches a response to fight it off. Normally, this response is proportionate and effective. With sepsis, the response becomes dysregulated. The 2016 Sepsis-3 consensus definition describes sepsis as “life-threatening organ dysfunction caused by a dysregulated host response to infection.”
In simpler terms, the body essentially starts attacking its own tissues in addition to the infection. Widespread inflammation is caused by chemicals released into the bloodstream to combat infection. Blood flow to vital organs, including the brain, heart, and kidneys, becomes compromised. If this progression is not stopped quickly with medical treatment, it can lead to septic shock, organ failure, and death.
Who Is at Higher Risk?
Sepsis can affect anyone, but certain groups face a significantly elevated risk:
- Adults 65 years of age and older
- Infants and children under one year of age
- People with weakened immune systems, including those with diabetes, cancer, kidney disease, or lung disease
- Individuals who are expecting or have just given birth
- Patients recovering from surgery, serious injury, or hospitalisation
- People who have previously survived sepsis
Being in one of these groups does not mean sepsis is inevitable, but it does mean that infections need to be treated promptly and monitored carefully.
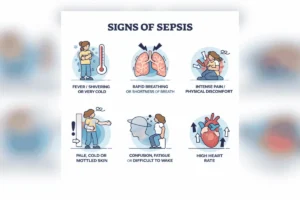
Common Symptoms of Sepsis
Sepsis can be hard to identify because its symptoms often resemble those of flu or a chest infection. The NHS advises calling 999 or going straight to A&E if an adult has any of these symptoms:
- Confusion, slurred speech, or disorientation
- Skin, lips, or tongue that are blue, grey, pale, or blotchy
- A rash that remains after rolling a glass over it
- Breathing problems or fast breathing
Other warning signs that warrant urgent medical attention include:
- Abnormally high or very low body temperature
- Rapid heart rate
- Severe shivering or chills
- Infrequent urination
- Swelling or unusual pain around a wound
It is worth noting that a person does not need to have all of these symptoms to have sepsis.
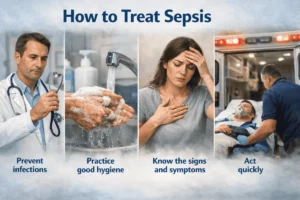
How to Treat Sepsis
Sepsis requires immediate medical care, and the earlier treatment begins, the better the outcome. According to Mayo Clinic, people with sepsis typically need to be monitored and treated in a hospital intensive care unit.
Treatment usually involves:
- Antibiotics: These are administered as soon as possible, often starting with broad-spectrum antibiotics before narrowing to target the specific infection.
- IV fluids: Intravenous fluids are given immediately to maintain blood pressure and support organ function.
- Oxygen: Many patients need supplemental oxygen, and in severe cases, mechanical breathing assistance.
- Vasopressors: If blood pressure remains dangerously low, medications to narrow blood vessels and raise blood pressure may be used.
- Surgery: In some cases, surgery is needed to remove infected tissue or drain pus from a wound.
How to Reduce the Risk of Sepsis
Since sepsis begins with an infection, reducing infection risk is the most effective prevention strategy. Practical steps include:
- Washing hands regularly and thoroughly
- Keeping cuts and wounds clean and covered until fully healed
- Staying current with recommended vaccines, including those for flu and pneumonia
- Managing chronic conditions like diabetes carefully
- Seeking medical attention promptly when an infection does not improve or appears to be getting worse
If you are already dealing with an infection and notice symptoms worsening rapidly, act quickly. The CDC advises asking a healthcare professional directly: “Could this infection be leading to sepsis?”
When to Seek Emergency Help
Sepsis moves quickly. A person who seems to have a manageable infection can deteriorate within hours. Do not wait to see if symptoms improve on their own; if any of the warning signs listed above appear, seek medical attention immediately.
Call emergency services or go directly to an emergency room if someone with an infection suddenly develops confusion, difficulty breathing, extreme weakness, a very rapid heart rate, or skin changes. Time is critical.
Protecting Yourself Starts With Understanding Sepsis
So, is sepsis contagious? No. Sepsis itself cannot pass from one person to another. It is not transmitted through touch, conversation, or shared spaces. When the body’s reaction to an infection gets out of hand, it becomes an internal medical emergency.
What can sometimes spread is the underlying infection that triggered it. This is why good hygiene, early treatment of infections, and staying informed about the warning signs all matter. Sepsis is a serious condition, but it is also one where early action can make a life-saving difference. The more people understand how it works, the better positioned they are to recognise it and respond quickly.




